Health Science | National Healthcareer Association (NHA) | CBCS
What Is the NHA CBCS Certification?
Being part of the AES curriculum team for over a decade, Kristin has experience in almost every aspect of the curriculum development process. She most enjoys problem solving, breaking down ideas, making connections for learners, graphic visualization, and typography.
As a health science curriculum developer, we work with thousands of teachers who need to prepare their students for industry certifications every year.
Many of these teachers are looking for ways to expand their offerings beyond medical assisting and CNA certifications.
One of the most popular options teachers consider when expanding their programs is the NHA Billing and Coding Specialist Certification (CBCS). But did you know the NHA has updated the CBCS exam?
If you’re starting a new medical billing and coding program or are planning your courses for next school year, you need to know the latest certification details!
On this page, you’ll discover how the exam is structured, what your students need to know, and how you can prepare students for success.
Before getting into the certification details, let’s recap what a medical billing and coding specialist is.
What Is a Medical Billing and Coding Specialist?
The NHA CBCS exam is an industry certification developed by the National Heathcareer Association (NHA). It’s designed to make sure medical professionals know how to properly code illnesses, procedures, and costs according to insurance standards.
According to the NHA, a billing and coding specialist may need to perform some or all of the following duties:
- Gather and review patient information
- Assign codes for diagnoses and procedures
- Verify documentation
- Submit claims reimbursements
- Prevent fraud
- Support coding and billing company-wide
- Educate health care providers
The skills learned through the NHA CBCS certification are essential to hospitals, physician offices, surgery centers, nursing homes, dental offices, home healthcare agencies, mental health facilities, and even insurance companies and consulting firms.
Obtaining a billing and coding specialist certification will open up extensive employment opportunities.
How is the NHA CBCS Exam Structured?
To be eligible for the NHA CBCS exam, students must have a high school diploma or GED equivalency as well as at least one of the following:
- Successful completion of a training program in the medical coding and billing field in the past five years
- At least one year of supervised work in coding and billing in the past three years
The NHA CBCS exam consists of 100 scored questions (plus another 25 pre-test questions used to gather data).
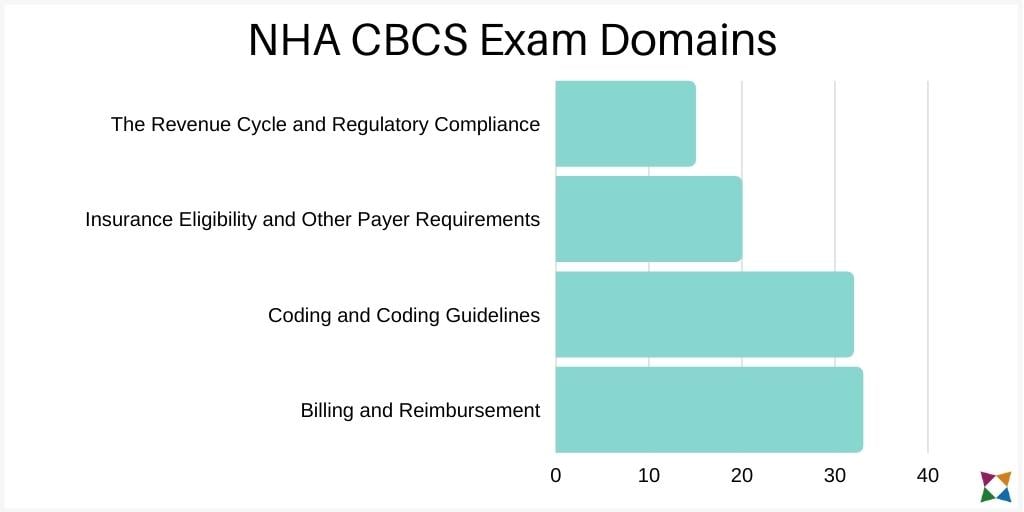
The questions fall into four topic areas, which NHA refers to as ‘domains’:
- The Revenue Cycle and Regulatory Compliance (15%)
- Insurance Eligibility and Other Payer Requirements (20%)
- Coding and Coding Guidelines (32%)
- Billing and Reimbursement (33%)
Each domain includes subtopics, categorized as either task statements or knowledge statements.
Task statements relate to physical duties that the student will need to know how to perform.
Knowledge statements refer to information and concepts that the student will need to know.
Continue reading to dive into the details of each domain.
Domain 1 - The Revenue Cycle and Regulatory Compliance
The Revenue Cycle and Regulatory Compliance domain includes 5 task statements related to revenue cycle concepts, the confidentiality of protected health information (PHI), compliance with regulatory law, and more.
The 9 knowledge statements are related to the phases of the revenue cycle, laws and regulations around PHI, permitted use or disclosure of PHI, and more.
To master this domain, students must confidently understand and apply the different revenue cycle concepts and understand their responsibilities around compliance.
Domain 2 - Insurance Eligibility and Other Payer Requirements
The Insurance Eligibility and Other Payer Requirements domain has 3 task statements related to verifying patient insurance information, eligibility of benefits, and differentiating among types of insurance plans.
The 11 knowledge statements relate to required insurance documentation, insurance eligibility, government insurance plans, patient financial responsibilities, and more.
To prepare for this domain, students should have a strong understanding of patient insurance eligibility and process.
Domain 3 - Coding and Coding Guidelines
The Coding and Coding Guidelines domain has 6 task statements related to applying knowledge of medical terminology, reviewing medical procedures and codes, identifying and applying the correct codes, and much more.
The 18 knowledge statements relate to a candidate’s knowledge of anatomy and physiology, medical terminology, standard medical acronyms, coding requirements, special considerations, and more.
To prepare for this domain, students should have a strong understanding of medical coding and terminology and understand how to apply this to the insurance process.
Domain 4 - Billing and Reimbursement
The Billing and Reimbursement domain has 13 task statements related to applying all applicable charges, transmitting claims electronically, determining financial responsibility, engaging in collection processes, and more.
The 19 Billing and Reimbursement knowledge statements measure knowledge of electronic claims submission processes, paper claims submission processes, the use of medical forms, reconsideration and appeals processes, aging report analysis, and more.
To master this domain, students should have a strong understanding of how to apply charges and bill patients appropriately and accurately.
For the full details of the exam, read the NHA Test Plan.
How to Prepare Students for the NHA CBCS Certification
Now that you know what’s on the NHA CBCS test plan, you’re probably wondering how best to prepare your students for the exam.
There are dozens of resources available to help you prepare your students for the CBCS exam, and many teachers are unsure of the best route to prepare their students for certifications.
Some teachers opt for the NHA test prep materials, while others add new curriculum resources like HealthCenter21 from AES to their program.
Each one has its own strengths and purpose within a health science certification program. Teachers even use them together to build a strong knowledge and skills base for students sitting for the NHA CBCS certification.
To determine which option would work best for your needs, dive into this article on the differences between test prep and health science curriculum:


